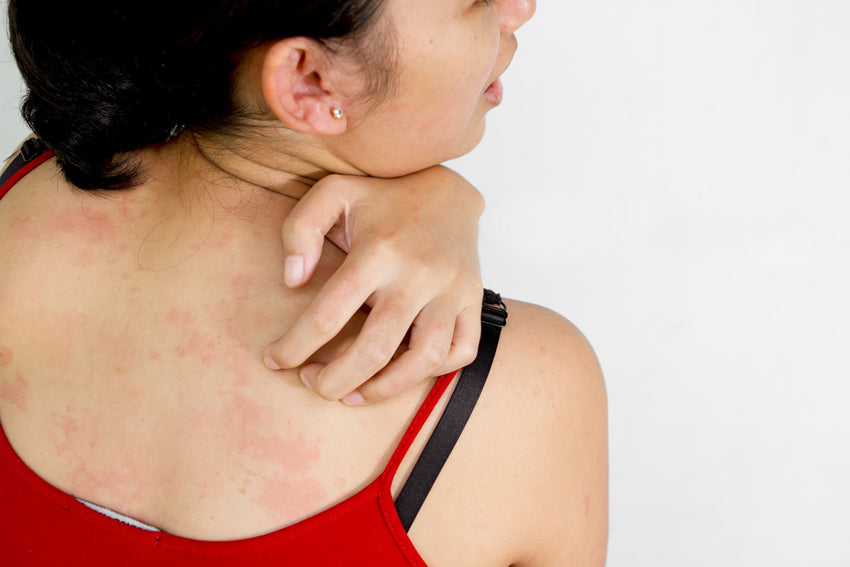
There are different types of blood tests for markers of inflammation, metabolic health and other indices, urine tests for metabolites, and different types of allergy testing (prick tests, skin tests, Intradermal (ID) testing, patch tests (usually for contact allergy). There is overlap between what dermatologists and allergists know and test for, however, IMO an allergist is going to know more about histamine and related disorders.
If she has a rash where her clothes or jewelry contact her, they would test for metals, detergents, dyes, fragrances, etc., and other things that contact her, and it may have little or nothing to do with food. There is also the timing of the food and rash and duration. These are things a good allergist would know. (A lot of this also depends on where the rash is, what it looks like, what it feels like, etc., and possibly other things in the medical history.)
Just to give you and idea (NOT medical advice!), here are 2 abstracts that talk a bit about histamine intolerance and food and "causing symptoms like diarrhea, hypotension, headache, pruritus and flush ("histamine intolerance"). Notice that it is not IgE mediated and skin-prick testing will typically be negative (according to the first source), so the allergist--if he agrees with the dermatologist-- could do other types of testing as I mentioned.
Clin Exp Allergy. 1993 Dec;23(12):982-5.
Histamine-free diet: treatment of choice for histamine-induced food intolerance and supporting treatment for chronic headaches.
Wantke F1,
Götz M,
Jarisch R.
Author information
Abstract
Histamine-induced food intolerance is not IgE-mediated. Skin-prick testing and specific IgE to food allergens are typically negative. Food rich in histamine or red wine may cause allergy-like symptoms such as sneezing, flush, skin itching, diarrhoea and even shortness of breath. The suspected reason is a diminished histamine degradation based on a deficiency of diamine oxidase. As diamine oxidase cannot be supplemented, a histamine-free diet was implemented to reduce histamine intake. Forty-five patients with a history of suffering from intolerance to food or wine (n = 17) and chronic headache (n = 28) were put on the diet over months to years. Fish, cheese, hard cured sausages, pickled cabbage and alcoholic beverages had to be avoided. Complaint intensity and drug-use per week prior to and 4 weeks after a histamine-free diet were compared. After 4 weeks on the diet 33/45 patients improved considerably (P < 0.01), eight of them had total remission. In 12/45 patients, however, no changes in symptoms were observed. Symptoms of food or wine intolerance significantly decreased (P < 0.02; treatment of choice), headaches decreased in frequency (P < 0.001), duration and intensity. After eating histamine-rich food symptoms were reproducible and could be eliminated by anti-histamines in most patients. These data indicate the role of histamine in food and wine intolerance and that histamine-rich food causes a worsening of symptoms in patients suffering from chronic headaches. Results obtained support the hypothesis of a deficiency of diamine oxidase in patients with intolerance to food or wine.
Comment in
PMID:
10779289
Allergy Asthma Proc. 2004 Sep-Oct;25(5):305-11.
Histamine intolerance-like symptoms in healthy volunteers after oral provocation with liquid histamine.
Wöhrl S1,
Hemmer W,
Focke M,
Rappersberger K,
Jarisch R.
Author information
Abstract
Histamine in food at non-toxic doses has been proposed to be a major cause of food intolerance causing symptoms like diarrhea, hypotension, headache, pruritus and flush ("histamine intolerance"). Histamine-rich foods such as cheese, sausages, sauerkraut, tuna, tomatoes, and alcoholic beverages may contain histamine up to 500 mg/kg. We conducted a randomized, double-blind, placebo-controlled cross-over study in 10 healthy females (age range 22-36 years, mean 29.1 +/- 5.4) who were hospitalized and challenged on two consecutive days with placebo (peppermint tea) or 75 mg of pure histamine (equaling 124 mg histamine dihydrochloride, dissolved in peppermint tea). Objective parameters (heart rate, blood pressure, skin temperature, peak flow) as well as a total clinical symptom score using a standardized protocol were recorded at baseline, 10, 20, 40, 80 minutes, and 24 hours. The subjects received a histamine-free diet also low in allergen 24 hours before hospitalization and over the whole observation period. Blood samples were drawn at baseline, 10, 20, 40, and 80 minutes, and histamine and the histamine-degrading enzyme diamine oxidase (DAO) were determined. After histamine challenge, 5 of 10 subjects showed no reaction. One individual experienced tachycardia, mild hypotension after 20 minutes, sneezing, itching of the nose, and rhinorrhea after 60 minutes. Four subjects experienced delayed symptoms like diarrhea (4x), flatulence (3x), headache (3x), pruritus (2x) and ocular symptoms (1x) starting 3 to 24 hours after provocation. No subject reacted to placebo. No changes were observed in histamine and DAO levels within the first 80 minutes in non-reactors as well as reactors. There was no difference in challenge with histamine versus challenge with placebo. We conclude that 75 mg of pure liquid oral histamine--a dose found in normal meals--can provoke immediate as well as delayed symptoms in 50% of healthy females without a history of food intolerance.
PMID:
15603203